Rural Healthcare Workforce
Maintaining the healthcare workforce is fundamental to providing access to quality healthcare in rural areas. Rural healthcare facilities must employ enough healthcare professionals to meet the needs of the community. They should have adequate education and training, skills to provide culturally competent care, and hold appropriate licensure or certification. When facilities promote coordination between health professionals and place them in roles where their skills can be used to best advantage, patients will receive the best possible care.
Strategies for optimizing the use of health professionals in rural areas include:
- Using interprofessional teams to provide coordinated and efficient care for patients and to extend the reach of each provider.
- Ensuring that all professionals are practicing to the full extent of their training and allowed scope of practice.
- Removing state and federal barriers to professional practice, where appropriate.
- Changing policy to allow expansions to existing scopes of practice if evidence shows that the healthcare workers can provide comparable or better care.
- Removing barriers to the use of telehealth to provide access to remote healthcare providers.
As the United States struggles with shortages of healthcare providers, an uneven distribution of workers means that shortages are often more profound in rural areas. This maldistribution is a persistent problem affecting the nation's healthcare system.
This guide examines policy, economics, planning challenges, and issues related to rural health workforce, including:
- Supply and demand
- Distribution of the workforce
- Characteristics of the rural healthcare workforce
- Licensure, certification, and scope of practice issues
- Programs and policies that can be used to improve the rural healthcare workforce
For additional information on rural healthcare workforce issues, see these RHIhub topic guides:
- Recruitment and Retention for Rural Health Facilities
- Education and Training of the Rural Healthcare Workforce
Frequently Asked Questions
- Is there a healthcare workforce shortage in rural areas?
- What is a Health Professional Shortage Area (HPSA)?
- How are HPSA designations determined?
- Where are HPSAs located in rural areas?
- What are Medically Underserved Areas (MUAs) and Medically Underserved Populations (MUPs)?
- How do the distribution and characteristics of the healthcare workforce compare across rural and urban areas?
- What state-level policies and programs can help address the problem of shortages in the rural healthcare workforce?
- What can schools do to meet rural healthcare workforce needs?
- What strategies can rural healthcare facilities use to help meet their workforce needs?
- How do international medical graduates help fill rural physician workforce gaps?
- Where can I find statistics on healthcare workforce for my state including employment, projected growth, and key environmental factors?
- What are some federal policies and programs designed to improve the supply of rural health professionals?
- Where can states get technical assistance for health workforce planning, including how to consider rural needs?
Is there a healthcare workforce shortage in rural areas?
Workforce shortages are very common in rural communities. It should be noted, however, that there is variation among rural communities when it comes to the adequacy of their health workforce supply. Some communities rarely experience health workforce supply problems, while others experience persistent shortages of health professionals.
The Council on Graduate Medical Education report Strengthening the Rural Health Workforce to Improve Health Outcomes in Rural Communities, published in 2022, noted that rural hospital closures have accelerated in recent years, and that workforce shortages are a problem even in areas that have retained their healthcare facilities. The report goes on to say that the COVID-19 pandemic has had the effect of exacerbating pre-pandemic shortages, leading to high levels of staff burnout, high turnover, and exposure to infection.
Whether shortages exist in rural communities and how severe they are can be difficult to determine since estimates of supply and demand for specific professions are not always available.
Maldistribution of healthcare professionals is also a problem affecting rural communities. The Association of American Medical Colleges document The Complexities of Physician Supply and Demand: Projections From 2019 to 2034 notes that if underserved populations had healthcare use similar to populations with fewer sociodemographic, economic, and geographic barriers, 102,400 to 180,400 additional physicians would be needed by 2034. Areas with higher proportions of residents from racial and ethnic minority populations or those who are economically disadvantaged, such as rural areas, tend to suffer most from lower supply of physicians and other health professionals.
The following factors were identified in an interview with WWAMI Rural Health Research Center researchers and in a National Rural Health Association policy brief:
- Education
- The current healthcare education system tends to be urban-centric.
- Access to healthcare training and education programs may be limited in rural areas, particularly beyond the community college level.
- Providers trained in urban areas may not be prepared for the challenges of working in rural communities or the kinds of health concerns rural patients may present.
- Urban areas frequently draw potential healthcare professionals away from rural areas. Students in rural communities may have to travel or relocate to an urban area for health professions coursework, unless they can find degree programs offered online, or for clinical training. Some do not return to rural communities after completion of their studies.
- There are fewer clinician role models in rural communities.
- Rural secondary school students may have fewer opportunities to receive the required math and science courses needed to pursue health careers.
- Rural Demographics and Health Status
- Rural populations usually have higher rates of chronic illness, which creates more demand.
- Rural areas tend to have higher proportions of elderly residents, who typically require more care.
- Rural populations tend to be poorer and may forego care due to cost.
- Rural Practice Characteristics
- When rural communities lack certain types of providers, particularly specialists, patients must travel longer distances or forego care if telehealth services are not available or an appropriate option.
- Barriers such as reimbursement policies and lack of broadband availability have hindered telehealth adoption in some rural areas. Many regulations related to telehealth have been relaxed or temporarily suspended, as a result of the COVID-19 pandemic. It remains to be seen whether these changes will remain in effect after the public health emergency ends.
- Rural communities may offer fewer opportunities for career advancement.
- Understaffing causes increased workloads, longer shifts, and less flexibility in scheduling, which may lead to healthcare provider burnout and be detrimental to the recruitment and retention of providers.
- Economics
- Urban facilities and practices may offer higher salaries, more benefits, and better working conditions.
- Health professions that require longer and more expensive training can be less affordable for rural students.
- Small, rural communities may offer fewer job opportunities for spouses, which can make recruiting providers difficult.
What is a Health Professional Shortage Area (HPSA)?
HPSA designations indicate shortages of healthcare professionals who provide primary care, dental, and mental health services. HPSAs are designated by the U.S. Health Resources and Services Administration (HRSA). A detailed description of HPSAs can be found at the HRSA Bureau of Health Workforce’s Types of Designations page. HPSAs may be:
- Geographic, based on the population of a defined geographic area
- Population-specific, for a subset of the population in a defined geographic area, such as those whose incomes are below 200% of the federal poverty level
- Facility-based, such as public or nonprofit private clinics, state mental health hospitals, and federal or state correctional facilities
In addition, there are safety net clinics that automatically receive shortage designation status. These include:
- Federally Qualified Health Centers (FQHCs) and FQHC Look-Alikes
- Indian Health Service and tribal clinics
- Rural Health Clinics (RHCs) – must complete a Verification of Clinic Data, CMS Form-29 that certifies the RHC meets all NHSC site requirements.
Maternity Care Target Areas (MCTA) are geographic areas within existing HPSAs that have shortages of maternity care professionals. Final criteria for MCTAs were published by HRSA in May 2022.
How are HPSA designations determined?
State Primary Care Offices are responsible for conducting needs assessments to determine which areas within their states should be considered shortage areas. They then submit applications to HRSA for review. For a fuller explanation of the process, see the HRSA Bureau of Health Workforce's Reviewing Shortage Designation Applications page. The primary factor used to determine whether a location may be designated as a HPSA is the number of full-time equivalent healthcare professionals relative to the population, with consideration given to high-need indicators such as a high percentage of the population living at or below 100% of the federal poverty level. See Scoring Shortage Designations for information related to the criteria and calculations HRSA uses to determine HPSAs.
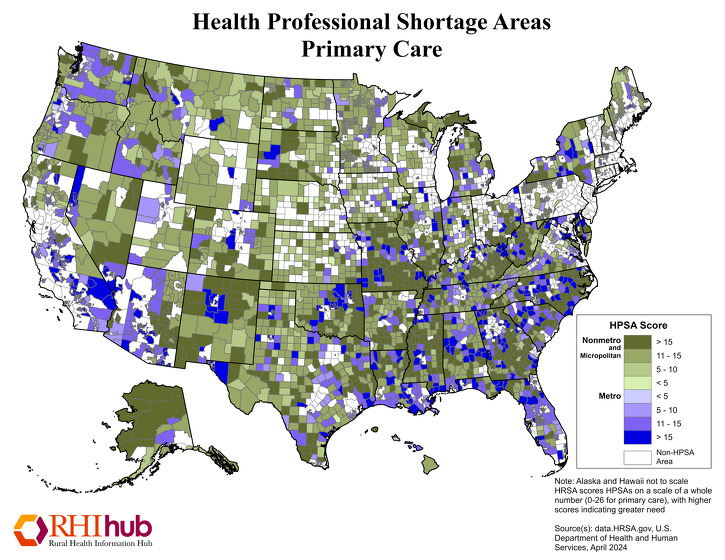
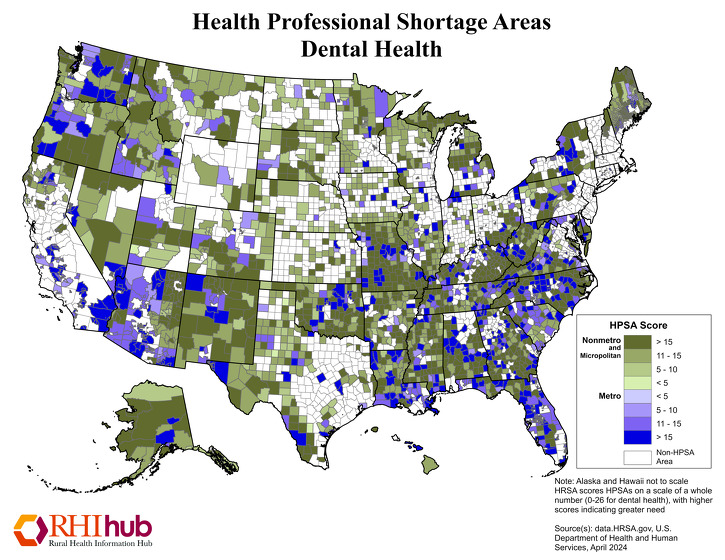
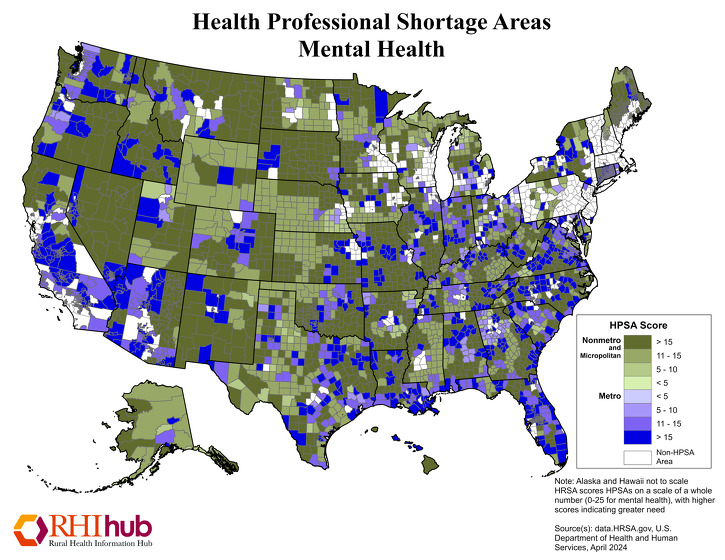
Where are HPSAs located in rural areas?
The following maps show designated HPSAs for primary care, dental health, and mental health, as of April 2024.
To search for HPSAs by state and county, see HRSA's HPSA Find tool. For statistics on HPSAs, including national percentages of HPSAs located in rural and urban areas, see the data.HRSA.gov Designated Health Professional Shortage Areas Statistics.
What are Medically Underserved Areas (MUAs) and Medically Underserved Populations (MUPs)?
Medically Underserved Areas (MUAs) and Medically Underserved Populations (MUPs) are federal shortage designations that indicate a lack of primary care services for an area or a population. MUAs and MUPs are based on four factors:
- Ratio of population to primary care providers
- Infant mortality rate
- Percentage of population below the federal poverty level
- Percentage of population age 65 or older
A list of MUAs and MUPs can be found at HRSA's Data Explorer. To search for MUAs and MUPs by state and county, visit HRSA's website, MUA Find.
For further information on MUA/MUP designations, see What is a Medically Underserved Area/Population (MUA/P)? on the HRSA website or contact your state Primary Care Office.
How do the distribution and characteristics of the healthcare workforce compare across rural and urban areas?
The following table shows ratios of health professionals per 10,000 population in rural areas as compared with urban areas for select professions. With the exception of Licensed Practical Nurses/Licensed Vocational Nurses, the supply of every type of health professional is lower in rural than urban areas:
| Occupation | Health professionals per 10K, Rural | Health professionals per 10K, Urban |
|---|---|---|
| Dentists | 4.7 | 7.6 |
| Registered Nurses | 63.9 | 95.3 |
| Licensed Practical Nurses/Licensed Vocational Nurses | 21.8 | 18.4 |
| Physician Assistants | 3.3 | 5.1 |
| Physicians (MDs) | 10.9 | 31.7 |
| Physicians (DOs) | 1.8 | 2.4 |
| Primary Care Physicians | 5.2 | 8.0 |
| Total Physicians | 12.7 | 33.6 |
| Nurse Practitioners | 8.4 | 10.4 |
| Total Advanced Practice Registered Nurses | 10.0 | 12.7 |
| Nurse Anesthetists | 1.3 | 1.8 |
| Physician data, 2020. Data for all other professions, 2021. (Source: HRSA Area Health Resources Files, 2021-2022.) | ||
Rural Primary Care Physicians
According to Figure 6 in the WWAMI Rural Health Research Center publication Supply and Distribution of the Primary Care Workforce in Rural America: 2019, non-core rural areas had more family physicians per 100,000 population than metropolitan or micropolitan areas, but fewer pediatricians and internal medicine specialists. The American Enterprise Institute document Nurse Practitioners: A Solution to America's Primary Care Crisis notes that between 2000 and 2016 the number of primary care physicians practicing in rural areas decreased by 15 percent, and this decline is expected to continue through 2030.
Rural Obstetrical Care Workforce
The WWAMI Rural Health Research Center's policy brief The Supply and Rural-Urban Distribution of the Obstetrical Care Workforce in the U.S. notes that rural areas have seen a decrease in access to maternal care in recent years, due in large part to closure of obstetric units and a shortage of healthcare professionals who deliver babies. Significantly fewer obstetricians serve nonmetro counties, per 100K women of childbearing age, compared to metropolitan counties. However, family physicians are more likely to deliver babies as the rurality of the county in which they practice increases.
| Occupation | Providers per 100K women of childbearing age, Metropolitan | Providers per 100K women of childbearing age, Nonmetropolitan |
|---|---|---|
| Obstetricians | 60.3 | 35.1 |
| Advanced Practice Midwives | 11.3 | 8.7 |
| Midwives | 5.2 | 5.6 |
| Family Physicians Who Deliver Babies | 9.8 | 34.4 |
| Source: The Supply and Rural-Urban Distribution of the Obstetrical Care Workforce in the U.S | ||
Rural Physician Assistants (PAs)
According to a June 2020 report from the WWAMI Rural Health Research Center, as of 2019 there were 24.1 PAs per 100,000 population in non-core counties, as compared with 32.3 in micropolitan areas and 42.5 in metropolitan areas. The same report notes that the number of PAs being trained is increasing at a higher rate than that of primary care physicians, indicating that numbers of PAs providing primary care in rural areas will continue to grow.
Rural Nurse Practitioners (NPs)
According to the same June 2020 report from the WWAMI Rural Health Research Center, as of 2019 there were 55.2 NPs per 100,000 population in non-core counties, as compared with 64.6 in micropolitan areas and 69.5 in metropolitan areas. Between 2010-2016 the NP workforce grew by 9.4%, thus increasing the number of NPs who might choose to work in rural areas.
Rural Certified Registered Nurse Anesthetists (CRNAs)
According to Understanding Advanced Practice Registered Nurse Distribution in Urban and Rural Areas of the United States Using National Provider Identifier Data, as of 2010 there were 0.9 rural certified registered nurse anesthetists (CRNAs) per 10,000 people, compared with 1.2 in urban areas. Male CRNAs were more common in rural areas, with 60.9% of rural CRNAs being male, compared with 38.5% of urban CRNAs. Among rural CRNAs, 66.8% practiced in large rural areas, 25.8% in small rural areas, and 7.3% in isolated small rural areas.
Rural Registered Nurses (RNs)
The 2021 Journal of Professional Nursing article Rural-Urban Differences in Educational Attainment Among Registered Nurses: Implications for Achieving an 80% BSN Workforce notes that urban nurses were more likely to have a BSN degree than rural nurses (57.9% versus 46.1%). In a survey of 34,104 nurses from all 50 states, the researchers found that rural nurses on average:
- Were slightly older than urban nurses (43.5 vs. 42.9 years)
- Had a shorter commute (22.9 vs. 24.4 minutes)
- Had lower salaries ($51,361 vs. $55,807)
The same study found that the majority of nurses work in hospitals, irrespective of rural or urban setting, and a higher percentage of rural nurses worked in skilled nursing facilities than urban nurses (12.7% versus 8.2%).
The 2017 HRSA report Supply and Demand Projections of the Nursing Workforce: 2014-2030 offers state-level projections for RNs and LPNs for the year 2030.
Rural Licensed Practical Nurses (LPNs)
According to a report from HRSA, The U.S. Nursing Workforce: Trends in Supply and Education (2013), rural LPNs are:
- About 24% of the LPN workforce – From 2008 to 2010, there were 690,000 LPNs in the nursing workforce. Of that number, 166,000 lived in rural areas. Thus, LPNs are disproportionately employed in rural areas.
- More likely to be White – 83.2% of rural LPNs are White, compared with 56.9% of LPNs in urban areas.
- Less likely to work for a hospital – 28.8% of LPNs working in rural areas are employed in hospitals, compared with 29.5% of urban LPNs.
- More likely to work in a nursing care facility – 33.5% of rural LPNs work in nursing care facilities, compared with 29.8% of urban LPNs.
- Same age as urban LPNs – The average age of both rural LPNs and urban LPNs is 43.6.
Rural Behavioral Health Professionals
The WWAMI Rural Health Research Center's report Changes in the Supply and Rural-Urban Distribution of Counselors in the U.S., 2014-2021 notes that there are only about two-thirds as many counselors per 100,000 population in rural U.S. counties than in metropolitan centers.
The following chart shows rates of providers in rural areas as compared with urban areas for selected behavioral health professions:
| Occupation | Providers per 100K, Metropolitan | Providers per 100K, Nonmetropolitan |
|---|---|---|
| Psychiatrists (2019) | 13.0 | 3.5 |
| Psychologists (2021) | 39.5 | 15.8 |
| Social Workers (2021) | 96.4 | 57.7 |
| Psychiatric Nurse Practitioners (2021) | 4.8 | 3.4 |
| Counselors (2021) | 131.2 | 87.7 |
| Sources: Changes in the Supply and Rural-Urban Distribution of Psychiatrists in the U.S., 1995-2019; Changes in the Supply and Rural-Urban Distribution of Psychologists in the U.S., 2014-2021; Changes in the Supply and Rural-Urban Distribution of Social Workers in the U.S., 2014-2021; Changes in the Supply and Rural-Urban Distribution of Psychiatric Nurse Practitioners in the U.S., 2014-2021; Changes in the Supply and Rural-Urban Distribution of Counselors in the U.S., 2014-2021, WWAMI Rural Health Research Center, 2022 | ||
What state-level policies and programs can help address the shortages in the rural healthcare workforce?
Funding options that states can use to address rural health workforce include:
- Supporting healthcare education and recruitment to rural areas through grants, loans, fellowships, scholarships, state loan repayment/forgiveness or scholarship programs, faculty loan repayment programs, tax benefits, and other incentives
- Increasing the number of healthcare graduates prepared for rural practice produced by state schools, by supporting the development and growth of healthcare education programs with rurally-oriented curricula
- Supporting rural clinical training opportunities, including residency programs
Policy options that states can use to address rural health workforce shortages include:
- Removing barriers to practice, such as allowing telehealth services to be provided across state lines
- Allowing new or alternative provider types to practice in rural areas
- Expanding existing scopes of practice
- Expediting licensure of new healthcare professionals and reactivation of expired licenses
What can schools do to meet rural healthcare workforce needs?
Health professions schools can:
- Use admissions criteria that are likely to produce providers interested in rural practice, such as admitting more students from rural communities or who intend to practice in a rural community
- Offer rural-centric curricula and training tracks
- Develop distance education programs
See RHIhub’s Education and Training of the Rural Healthcare Workforce for more information.
What strategies can rural healthcare facilities use to help meet their workforce needs?
Rural healthcare facilities can employ various strategies to ease healthcare workforce shortages and improve care. For instance, they can use technology, such as telehealth, to fill gaps in care caused by shortages. In addition, facilities can use interprofessional care teams to provide more efficient and high-quality care and can participate in educating rural healthcare professionals through offering clinical training experiences.
Redesigning practice and processes to allow professionals to work at the top of their license and skill set can also lessen the effects of shortages. Facilities can provide workers with opportunities to learn new skills and encourage them to pursue career advancement through apprenticeships and other educational opportunities.
Rural areas often experience difficulties related to recruitment and retention of primary care and other health professionals. Thus, it is important to plan for future workforce needs. By anticipating retirements and departures of staff, administrators can take steps to recruit replacements in a timely manner, and avoid prolonged vacancies at their facilities. Increasing pay, benefits, flexibility, and opportunities for career advancement can also improve chances for success with recruitment and retention.
For ideas on recruiting and retaining healthcare professionals, see RHIhub's Recruitment and Retention for Rural Health Facilities guide.
How do international medical graduates help fill rural physician workforce gaps?
Many rural communities recruit international medical graduates with J-1 visa waivers to fill physician vacancies. The Conrad State 30 Program allows each state's health department to request J-1 Visa Waivers for up to 30 foreign physicians per year. The physicians must agree to work in a federally designated Health Professional Shortage Area (HPSA) or Medically Underserved Area (MUA). Interested parties should contact the Primary Care Office in the state where they intend to work, for more information and exact requirements. See RHIhub's Rural J-1 Visa Waiver topic guide for details.
In addition to the J-1 visa waiver, non-immigrant H-1B visas are sometimes used to fill employment gaps. These are employer-sponsored visas for “specialty occupations,” including medical doctors and physical therapists. H-1B visas are issued for three years and can be extended to six years. For more information, see the U.S. Citizenship and Immigration pages on the H-1B Program and H-1B Specialty Occupations.
Where can I find statistics on healthcare workforce for my state, including data on employment, projected growth, and key environmental factors?
HRSA's National Center for Health Workforce Analysis provides in-depth data on supply, demand, distribution, education, diversity, and use of health personnel. State level profiles are available, which provide data for 35 types of health workers including physicians, nurses, and dentists.
The National Forum of State Nursing Workforce Centers provides a list of state nursing workforce center initiatives throughout the nation.
HRSA's Area Health Resources Files (AHRF) provides demographic and training information on more than 50 healthcare professions.
The U.S. Department of Labor's Occupational Employment Statistics: May 2021 State Occupational Employment and Wage Estimates provides state-level information on occupational employment within “Healthcare Practitioners and Technical Occupations” and “Healthcare Support Occupations.”
The Association of American Medical Colleges (AAMC)'s 2021 State Physician Workforce Data Report provides data on physician supply, medical school enrollment, and graduate medical education throughout the United States. AAMC's Physician Specialty Data Report, published biennially, provides statistics on active physicians and physicians in residency and fellowship programs for 48 specialty groups.
The Kaiser Family Foundation's State Health Facts: Providers & Service Use Indicators provides data on physicians, RNs, PAs, NPs, dentists, and healthcare employment.
The Robert Graham Center's Workforce Projections provides primary care physician workforce projection reports for all states.
What are some federal policies and programs designed to improve the supply of rural health professionals?
Area Health
Education Centers (AHEC) Program
AHECs promote interdisciplinary, community-based training initiatives intended to improve the diversity,
distribution, supply, and quality of healthcare personnel, particularly in primary care. The emphasis is on
delivery sites in rural and underserved areas. AHECs act as community liaisons with academic institutions and
assist in arranging training opportunities for health professions students, as well as K-12 students.
Health Careers Opportunity Program (HCOP)
HCOP works to increase the number of people from economically disadvantaged backgrounds who enter the health
professions field. HCOP programs provide student stipends and financial support to attend health professions
schools, training for disadvantaged students, and counseling and mentoring services to help students complete
their education and training. Students are exposed to community-based primary healthcare experiences.
National Health Service Corps (NHSC)
NHSC offers scholarships and loan repayment programs, which can enable students to complete health professions
training. Students must agree to complete a service commitment in a Health Professional Shortage Area. According
to the infographic Building
Healthier Communities, approximately 1 in 3 NHSC clinicians works in rural areas. This represents
more than 3,000 primary care clinicians, more than 3,400 clinicians working in the areas of mental and
behavioral health,
and almost 700 dental clinicians.
Teaching Health Center Graduate Medical Education (THCGME)
Program
The THCGME program supports students in primary care residency training programs in community-based ambulatory
patient care centers. There are two types of awards: Expansion awards for an increased number of resident
full-time equivalent positions at existing HRSA THCGME programs and new awards to support new resident FTE
positions at new Teaching Health Centers.
Teaching Health Center Planning and Development (THCPD)
This program makes awards to establish new accredited community-based primary care medical or dental residency
programs and residency programs to address shortages in the primary care physician and dental workforce
shortages and challenges faced in rural and underserved communities.
Rural Residency Planning and Development (RRPD) Program
The RRPD program provides funding to create new rural residency programs. Grants of up to $750,000
are provided to cover direct and indirect costs for accreditation, faculty development, and resident
recruitment.
Where can states get technical assistance for health workforce planning, including how to address rural needs?
The Health Workforce Technical Assistance Center (HWTAC) offers technical assistance to states and organizations involved in health workforce planning. HWTAC activities can include:
- Direct technical assistance
- Educational webinars
- Facilitating access to health workforce data
HWTAC is a partnership of the Center for Health Workforce Studies (CHWS) at the School of Public Health, University at Albany, State University of New York and the Cecil G. Sheps Center for Health Services Research at the University of North Carolina. It is funded by HRSA's National Center for Health Workforce Analysis.